Our expert gynecologic oncologists care for patients compassionately to offer the best possible chance for cure with the best possible quality of life. Our team focuses on decreasing toxicity and protecting quality of life with fertility-sparing surgical techniques, as well as sentinel lymph node biopsies.
Cervical cancer patients find comfort in our personalized, holistic, and warm approach to care. In addition to access to experts at a leading academic medical center, our patients also benefit from greater access to their attending physician, video visits, e-message, flexible scheduling, and collaborative care with a wide range of specialists.
Cervical cancer is a type of cancer that begins in the cervix, the part of the uterus that opens into the vagina or birth canal. It is the only gynecologic cancer that can be prevented with regular screening and a preventative vaccine.
Cervical cancer is caused by abnormal cell growth in the two main types of cervical cells:
Cervical cancer is caused by the human papillomavirus (HPV), a common virus that is spread during sex. For most women, HPV goes away over time. Women have a higher risk for cervical cancer if they have persistent HPV, smoke, have HIV, use birth control pills for more than five years, have given birth to three or more children, or have multiple sexual partners.
The HPV vaccine protects against the HPV virus that causes cervical cancer. Typically, the HPV vaccine is given to preteens. In addition, quitting tobacco use and limiting the number of sexual partners helps prevent cervical cancer.
Two screening tests help detect cervical cancer:
HPV test
Cervical precancers typically do not cause symptoms. Once cancerous cells have developed, the most common symptoms include:
Our physicians first perform a general physical and pelvic exam. If cervical cancer is suspected, you may undergo an HPV test or a biopsy.
If cancerous cells are found, this represents a diagnosis of cervical cancer. It is important that you seek out care from highly trained gynecologic oncologists for targeted, personalized treatment and care.
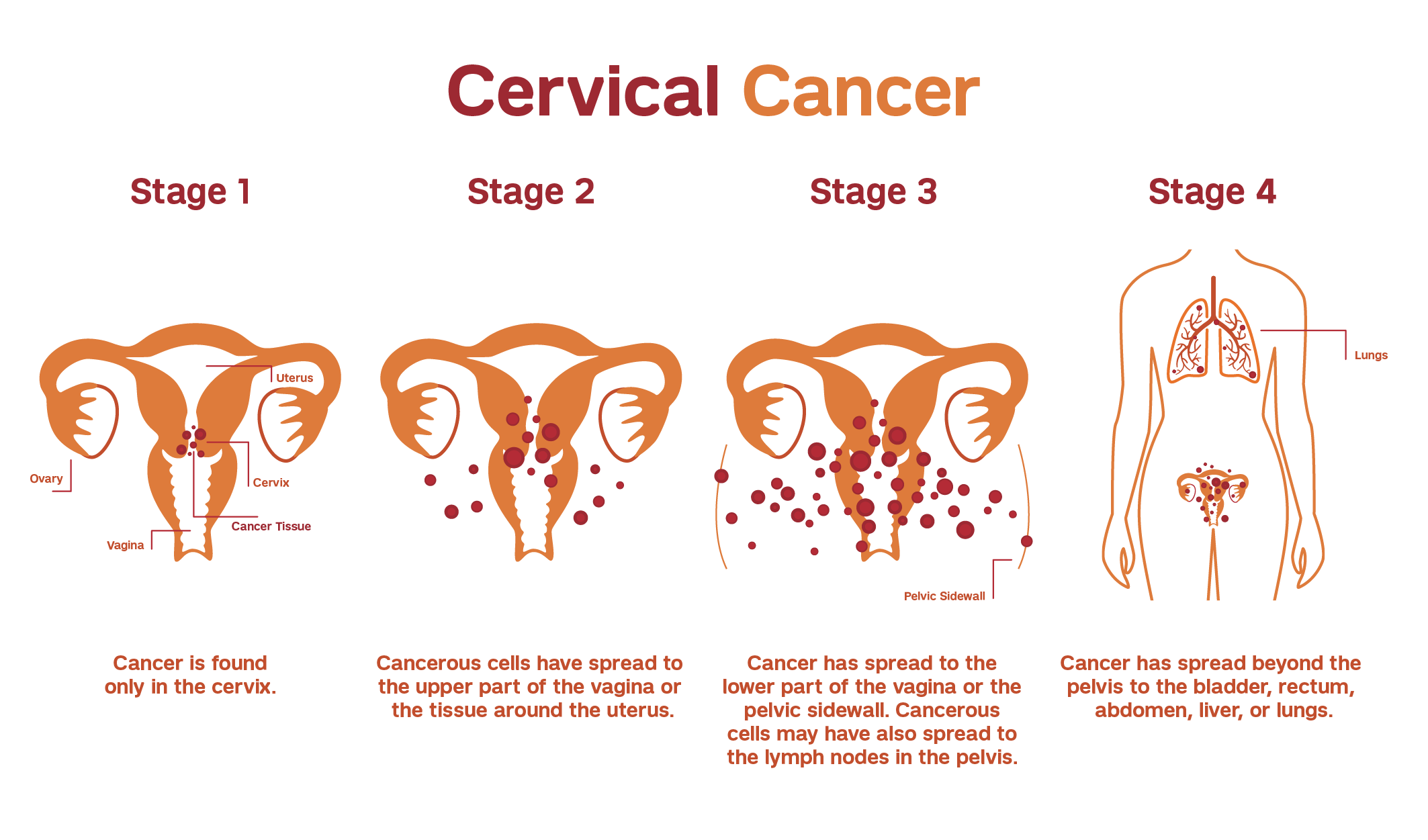
It is critical to determine if and where the cancer is and the extent of disease. Our team of expert gynecologic oncologists carefully evaluate each patient to determine the stage of cervical cancer and develop a personalized treatment plan.
A PET MRI scan helps determine the stage without radiation exposure. Surgery may be recommended to better determine the stage.
Our team of gynecologic oncologists personalize treatment depending on many factors, including cervical cancer stage and fertility goals.
Individual treatment plans may include a combination of surgery, radiation therapy, chemotherapy, immunotherapy, and other treatment options. Our physicians work closely with patients to minimize side effects and promote greater comfort throughout treatment.
If precancerous cells are detected our gynecologic oncologists can surgically remove them with laser ablation and conization to remove only the cancerous parts of the cervix. These treatments can protect fertility.
Other options include cryotherapy (chemically freezing cancerous cells to remove them from the cervix) and Loop Electrosurgical Excision Procedure (LEEP) biopsy (a small electrical wire is used to remove cancerous cells from the cervix).
At Weill Cornell Medicine, our gynecologic oncologists are highly trained surgeons who tailor surgical treatments to the patient’s unique needs and goals. Surgical options may include:
Our gynecologic oncologists work closely with expert radiation oncologists at Weill Cornell Medicine to treat appropriate cervical cancer patients with radiation therapy.
Chemotherapy is the use of drugs to kill cancerous cells. To limit side effects and damage to healthy cells, cervical cancer patients are usually given chemotherapy in cycles with several rest periods.
Women may receive intravenous chemotherapy after surgery, in combination with radiation, for the treatment of recurrent cancer. Our expert gynecologic oncologists determine the most effective combination of drugs for each patient depending on a variety of factors.
Our patients benefit from Weill Cornell Medicine’s state-of-the-art chemotherapy treatment center, which provides unique support and resources.
Immunotherapy is the use of medications to stimulate your immune system to recognize and destroy cancer cells more effectively. Your physician determines the best immunotherapy medications and timing for taking them.
With care from a highly trained gynecologic oncologist, immunotherapy can be an integral part of your cervical cancer treatment.
Our gynecologic oncologists work closely with the expert reproductive medicine specialists at Weill Cornell Medicine to offer cervical cancer patients options to preserve fertility, including radical trachelectomy and egg or embryo freezing.
The gynecologic oncologists at Weill Cornell Medicine collaborate with other specialists and researchers within the cancer center to offer unparalleled interdisciplinary care at our top-ranked hospital.
Weill Cornell Medicine patients have access to specialists in gynecology, surgical oncology, medical oncology, pathology, radiation oncology, genetics, nutrition, social work, and reproductive medicine. In addition, our patients benefit from collaborative care with:
Our gynecologic oncologists and physician assistants work closely with patients to promote wellness during and after treatment – with the goal of helping you return to the full breadth of functional living you enjoyed before the diagnosis. Our team provides frequent follow-up care and monitoring for recurrence.
In addition, we will connect you with support groups, services, and resources to live as fully as possible.