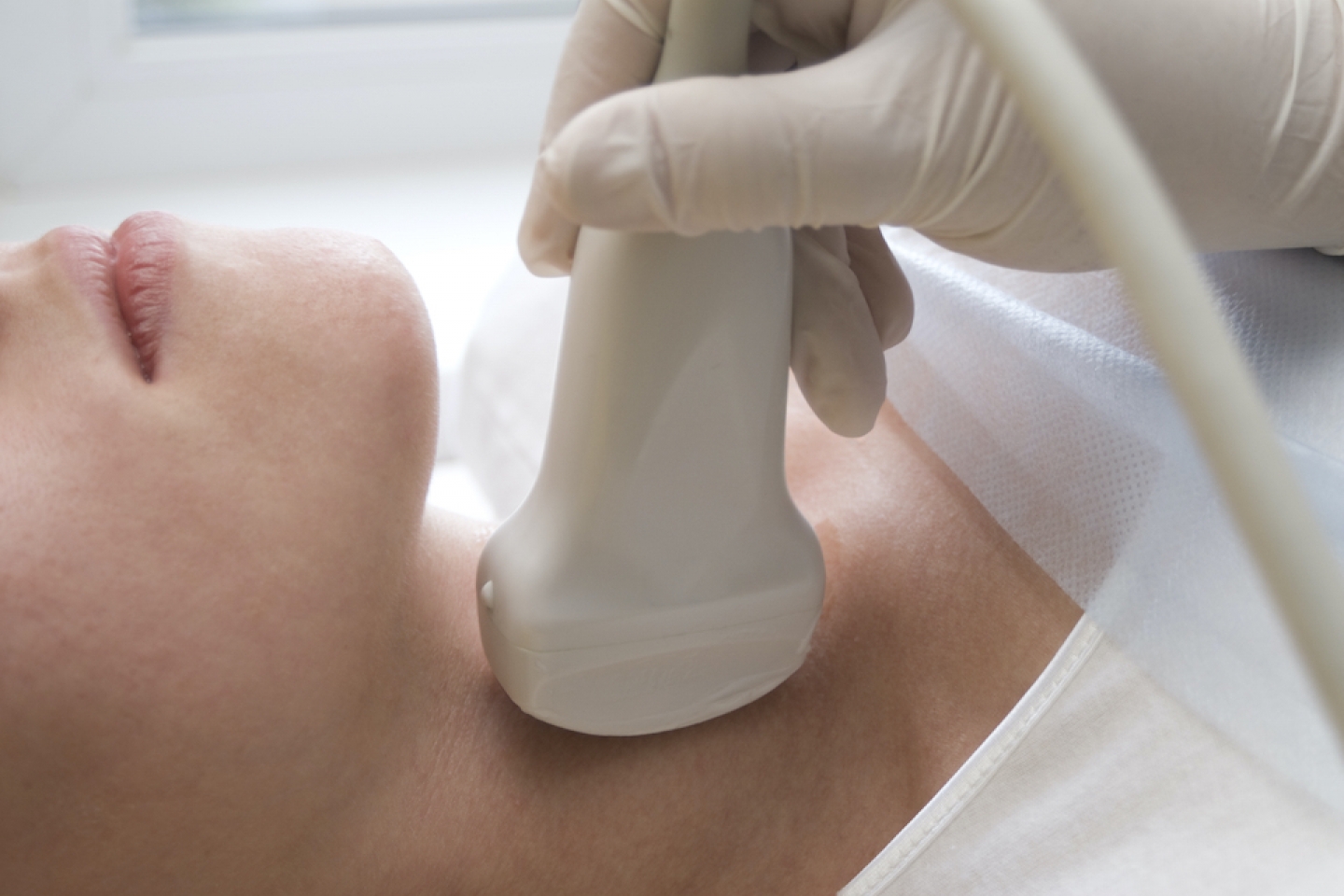
If you have unusual swelling at the front of your neck, palpitations, insomnia, fatigue, unexplained weight gain or loss, diarrhea, or constipation, you could have thyroid disease.
More than 12 percent of the U.S. population will experience a thyroid condition at some point in their lives, according to the American Thyroid Association (ATA). One in eight women will also develop a thyroid disorder during their lifetime. In fact, women are five to eight times more likely than men to have thyroid problems, especially following pregnancy and menopause, the ATA says.
Yet, thyroid disease often goes undetected: as many as 60% of people don’t know they have it, which is why regular screening is important.
The thyroid is a small gland at the front of your neck that makes the thyroid hormone that regulates your metabolism, says Dr. Thomas J. Fahey III, Chief of Endocrine Surgery, and Director of the Endocrine Oncology Program. “The thyroid has a wide-ranging effect throughout the body. It contributes to how fast your heart beats, how fast your hair grows, and how fast things pass through your intestines,” Dr. Fahey says.
The thyroid gland commonly malfunctions, typically by over- or under-producing hormones. An over-functioning thyroid gland can trigger “hyperthyroidism,” which can cause your body to race and your heart to pound, as well as weight loss, sleep trouble, muscle weakness, frequent or loose bowel movements, nervousness, or irritability. The most common cause of hyperthyroidism in the U.S. is Graves' disease, an autoimmune disorder in which the immune system attacks the thyroid gland. An under-functioning thyroid, which frequently stems from the autoimmune disorder Hashimoto’s disease, may lead to “hypothyroidism” and resulting fatigue, weight gain, depression, constipation, heavy or irregular menstrual periods, or problems conceiving. Family history increases the risk for both Hashimoto’s and Graves’.
According to Dr. Fahey, if you live long enough, then you’re likely to develop thyroid nodules, solid or fluid-filled lumps within the thyroid gland. Most of the time, these nodules are harmless and produce no symptoms. “A nodule can be deemed to be malignant, which is the least common outcome, while approximately 25%-30% of the time it is ‘indeterminant,’ which means it contains slightly unusual cells that aren’t necessarily cancerous,” Dr. Fahey explains. “In such situations, your doctor will send these cells out for further testing, and then decide to either continue observing the nodule or remove it if it is found to be cancerous.”
If nodules grow large enough, or impede breathing or swallowing, however, they can threaten your health. Nodules that are cystic are less worrisome than those that are solid, Dr. Fahey says. Yet, a cystic nodule that exceeds two centimeters, or a one-centimeter solid nodule, will likely require a fine needle biopsy so your doctor can rule out thyroid cancer. Your doctor may also order blood work, a thyroid function test, and an ultrasound to see if a nodule is solid, cystic, or both.
Fortunately, thyroid cancer is generally very treatable and curable, often with neck surgery and some additional treatment, including radioactive iodine therapy for more aggressive tumors that require removing the entire thyroid. This surgery, which is often done on an outpatient basis, can take one to three hours. “Recovery is not usually difficult, and patients typically do very, very well,” Dr. Fahey says.
Immediately following surgery, patients will have one or two follow up visits with their oncologist, as well as an ultrasound and bloodwork every six months, and yearly afterward.
Treatment advances for thyroid cancer patients, including tyrosine kinase inhibitors that target the mutations found in the cancer and have the ability to stabilize it, offer a bright future, Dr. Fahey notes. “There is overall a very optimistic outlook for the treatment and management of patients with thyroid cancer,” he says.