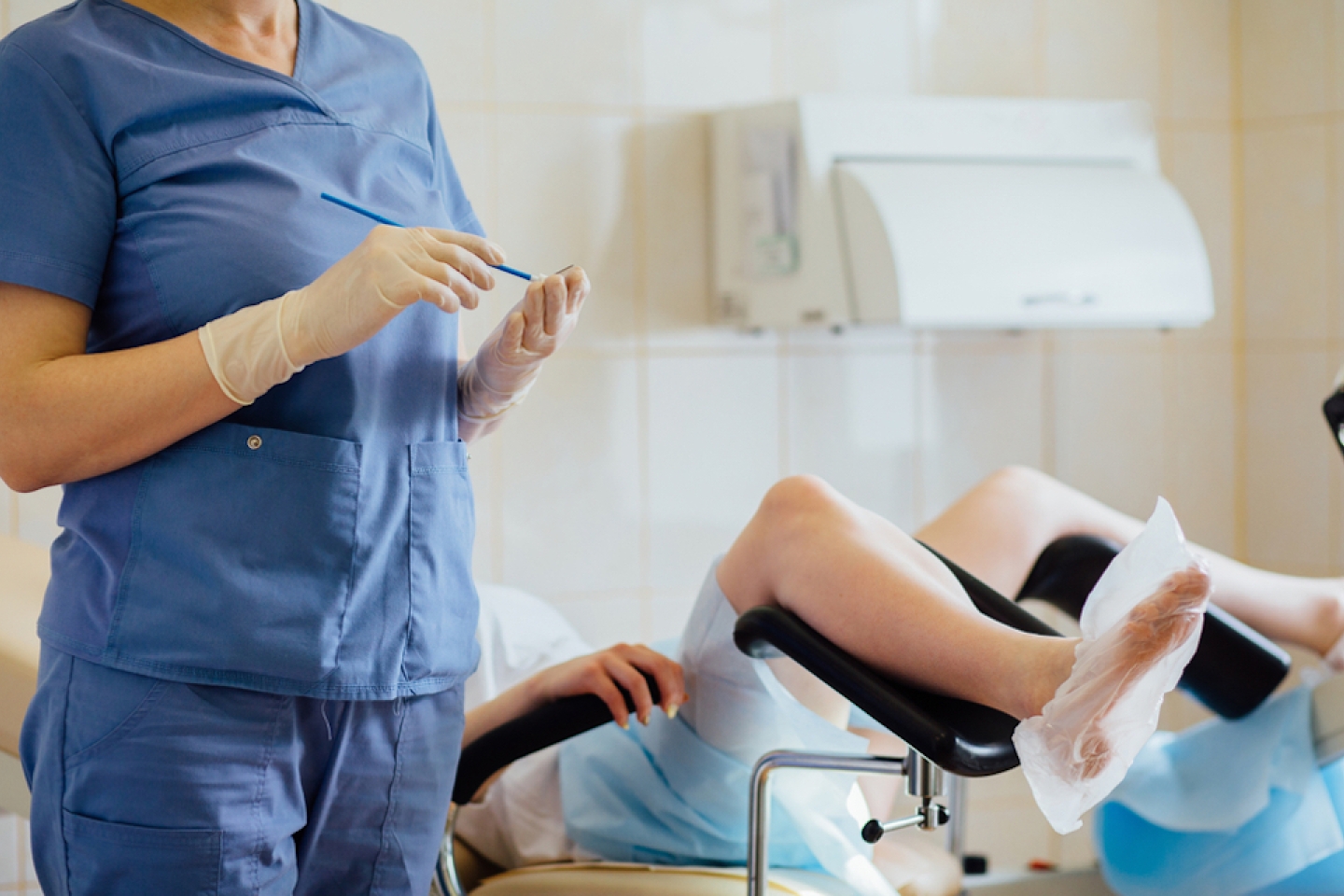
The Pap smear, a routine part of a woman’s annual visit to her gynecologist for nearly 100 years, was developed at Cornell University Medical College by Dr. George Papanicolaou in 1928. The test has been used ever since to screen women for precancerous or cancerous changes to the cervix: the lower, narrow end of the uterus.
“The Pap smear helps to prevent a cancer just through screening,” says Dr. Eloise Chapman, a gynecologic oncologist and division director of gynecologic oncology at Weill Cornell Medicine. “It continues to protect women from cervical cancer to this day.”
During January—Cervical Cancer Awareness Month—patient education is key, Dr. Chapman says. As well, health-care providers need to do their utmost to broaden access to care, especially to lower-income women of color.
All the elements of cervical cancer prevention are there, she says, with one exception: The U.S. does not have a comprehensive HPV (human papilloma virus) vaccination program comparable to those that have been adopted by other developed countries. HPV is known to cause cervical cancer, and the vaccine effectively blocks HPV infection. It’s available in this country, and it can be given to both boys and girls starting at ages 11 to 12 or even as young as 9.
Why include boys? Because HPV is transmitted through sexual contact. The idea is to vaccinate children of both genders before they become sexually active. “By preventing infection from occurring in the first place, the vaccine can dramatically reduce the risk of cervical cancer later in life,” says Dr. Evelyn Cantillo, a gynecologic oncologist and assistant professor of obstetrics and gynecology at Weill Cornell Medicine. “In other countries, vaccination is doing just that: creating herd immunity as a key strategy in prevention.”
Cervical cancer is the third most common reproductive cancer diagnosis in the U.S., Dr. Cantillo says, which is why we need a vigorous HPV vaccination program in this country.
The first level of screening takes place during your annual visit to the gynecologist’s office or when you see your primary care physician (PCP) who does gynecological exams. Starting at age 21, as long as you are not immunocompromised, you’ll undergo your first Pap smear. And at age 30 or so, you’ll have an HPV test, which assesses your cervical cancer risk over a 5-year period.
The DNA-based HPV test checks for specific high-risk HPV subtypes that are linked to 80 to 90 percent of cervical cancers. “If you don’t have these,” Dr. Cantillo says, “it’s highly unlikely that you’ll develop cervical cancer in the next 5 years.”
Women under 25 typically clear the virus on their own through natural immunity. But about 20 percent of them may go on to have precancerous lesions and, ultimately, cancers. “In women 30 and above, we do a Pap smear plus an HPV test. That combination helps us identify women we need to follow more closely and those who are at lower cancer risk,” she says.
If a patient’s Pap smear and HPV test both indicate higher risk, “we do a procedure called a colposcopy to examine the cervix more closely and perform one or more biopsies if needed,” Dr. Chapman says. “If we find something to treat, we can get rid of it very easily with small surgical incisions so that it never develops into cancer.”
If she finds a tumor on the cervix that is less than 2 cm and the cancer hasn’t spread, Dr. Chapman treats it surgically. But once it has spread, surgery is off the table. “If we succeed in finding the cancer early, we can potentially avoid major surgery that can cause a woman to lose her fertility. We can remove the abnormal portion of the cervix, by doing a larger biopsy of the cervix called a cold knife conization, or removal of entire cervix (trachelectomy) allowing us to protect fertility. For tumors larger than 2cm, surgery may still be an option but usually involves removing both the uterus and the cervix.
“If the cancer is large or has spread beyond the cervix to the other reproductive organs,” she continues, “we administer chemotherapy and radiation therapy at the same time. And if it has spread from the reproductive organs to other parts of the body, we just use chemotherapy—and hope for a cure.”
To preserve fertility, Dr. Chapman brings in a reproduction endocrine infertility team to freeze the woman’s eggs within a week and a half of diagnosis. Then, she can go right into treatment.
If the cancer is found early, there are surgical procedures that can be done to preserve the uterus, while only removing the cervix, and biopsy lymph nodes.
And if the patient receives a cancer diagnosis while already pregnant, Dr. Chapman and her colleagues focus on getting her through her pregnancy and delivering her baby. Then, after delivery, the patient goes into treatment immediately.
Reducing health disparities and fostering prevention are at the heart of Dr. Chapman’s work at Weill Cornell Medicine. She is committed to educating patients on the benefits of HPV testing and vaccination, as well as preventive procedures like colposcopy. Countering misinformation is a major goal in her practice and her research.
She relies on a system invented at Weill Cornell Medicine called PALS, which stands for Patient-Activated Learning System. Harnessing the power of text messaging and email, Dr. Chapman communicates directly with patients, often as part of her follow-up after an abnormal Pap smear. “A big risk factor for cervical cancer is having a Pap smear and not following up,” she says. “PALS helps us eliminate that risk factor.
“It’s amazing that you can get screened and have a vaccine and prevent a cancer,” she adds. “Cervical cancer is highly preventable. Patients need to know their options and work with us to cut their cervical cancer risk down to size.”
To make an appointment for cancer screening with a gynecologist or reproductive oncologist at Weill Cornell Medicine, please visit here.