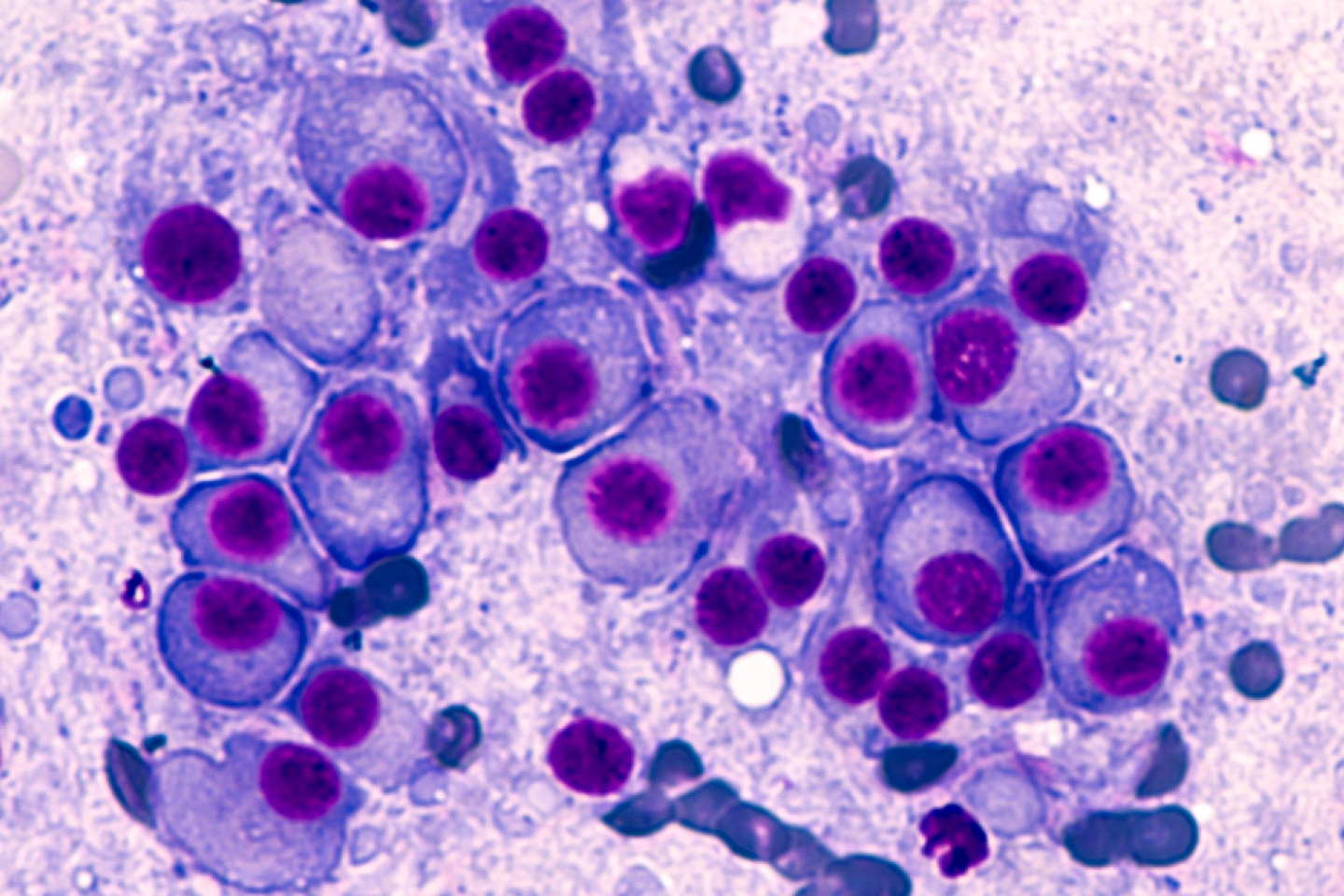
Blood cancer is not one disease but many. Let’s focus on one: multiple myeloma. The second most common blood cancer, multiple myeloma (MM) is a cancer of plasma cells in our bone marrow, where all blood cells are made.
Plasma cells are the white blood cells in charge of making antibodies to fight infections, says Dr. Jorge Monge, an assistant professor in the division of hematology and medical oncology at Weill Cornell Medicine and assistant attending physician at NewYork-Presbyterian Hospital. “When these cells acquire mutations and become cancerous, they grow in number and produce an excess of abnormal antibodies,” he explains.
True to its name, MM can cause harm in multiple ways.
While the cause of MM is unknown, says Dr. Monge, “exposure to radiation or to certain insecticides, herbicides or chemicals such as benzene may play a role. As well, exposure to dust and other particulates at the World Trade Center disaster site, especially in the first year after the towers fell, is believed to be associated with the development of MM or one of its possible precursors: smoldering multiple myeloma, for one, or MGUS—an abbreviation for monoclonal gammopathy of undetermined significance.
If blood tests show evidence of abnormal antibodies but none of the damaging effects listed above are present, specialists label the condition “smoldering multiple myeloma”—in other words, MM that is asymptomatic.
Says Dr. Monge, “There are tests that can help predict a patient’s risk of progressing from smoldering MM to ‘active’ MM. If the risk of progression is very high, we now call it ‘active’ MM and start treatment before it can cause damage.”
But not all asymptomatic cases rise to the level of an MM diagnosis, even a smoldering one. Sometimes, abnormal plasma cells do not show up at sufficiently high levels in the bone marrow to warrant such a diagnosis, Dr. Monge says, and these cells produce only a small number of abnormal antibodies. Labeled MGUS, that condition is not considered cancer at all: “Only 1 percent of people with MGUS will develop cancer from year to year.”
For reasons that are poorly understood, MM is 1.5 times more common in men than women, and twice as common among people of African American descent than among whites. It is most often diagnosed in patients between 65 and 74 years old.
About 160,000 people are living with MM in the U.S., and an estimated 34,000 new cases will be diagnosed this year.
When MM is first suspected, a blood test can detect the abnormal antibodies associated with the disease. To look for any damage to the body, other tests can be performed, including blood, urine and imaging tests such as X-rays, a CT scan or a PET scan. When appropriate, a bone marrow biopsy should be done to confirm the diagnosis. The biopsy will also facilitate genetic testing to assess a patient’s risk for developing more aggresive disease.
“Based on national data from 2018, 58 percent of patients survive 5 years or longer after an MM diagnosis,” Dr. Monge says, “and that number continues to increase each year, thanks to new treatments and improvements in supportive care.”
Initial treatment, he says, includes multiple drugs; how we combine them depends on the person’s health and age. Patients who are candidates for a stem cell transplant are treated beforehand with a 3- or 4-drug combination of a steroid, a proteasome inhibitor, an immunodulatory drug and a monoclonal antibody. “With the ongoing development of new treatment combinations, more than 90 percent of patients respond to initial therapy,” he says.
Patients who are not candidates for stem cell transplant can receive a lower-intensity combination designed to avoid side effects and still show an improvement in survival.
To learn more about multiple myeloma and its “precursor” conditions—smoldering MM and MGUS—or to make an appointment at Weill Cornell’s Myeloma Center, visit here.