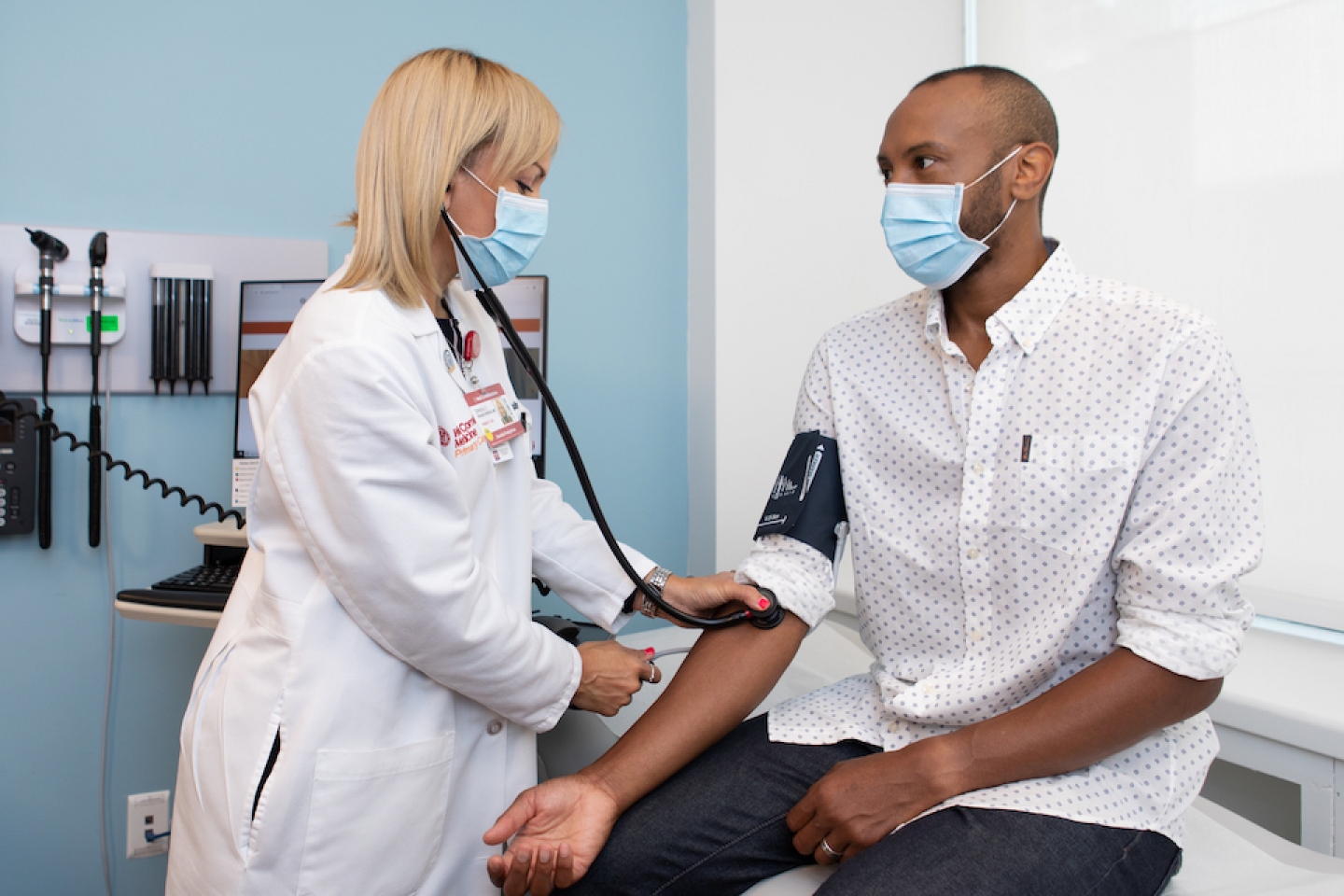
Did you know that men are more likely than women to have chronic diseases but less likely to see a doctor for checkups or preventive care?
Men’s Health Month began in 1992 to urge men to pay closer attention to their health, particularly to chronic conditions that--with proper screening--are treatable and even preventable, according to Benjamin Scallon, MD. “We know that men seek out medical care less frequently than women, for both preventative services and sick visits,” Dr. Scallon says. “There are many complicated reasons why, ranging from a gendered masculine script of independence and resilience to nongendered-specific reasons, such as not wanting to take time away from work.”
Whatever the reasons, ignoring their overall health or worrisome symptoms that could indicate underlying health problems, increases a man’s risk for illness and early death.
Cardiovascular disease, preventable cancers, and mental health issues are the greatest health risks for both women and men. Because heart and vascular diseases are the leading causes of death in adults, men should seek screening and treatment for related chronic conditions--that are easy to ignore--such as obesity, high blood pressure, high cholesterol, and diabetes, Dr. Scallon says. “Men often see me for help with erectile dysfunction, often not realizing it can be associated with heart and vascular disease,” he says. “It is important for men to maintain a heart-healthy lifestyle by not smoking, eating a healthy diet, and exercising.”
Screening for anxiety and depression is also important, especially since men are much less likely than women to seek care for mental health issues,” Dr. Scallon says. “The reasons why men do not seek out care probably include a ‘pick yourself up by the bootstraps’ mentality, as well as persistent stigma towards mental health in our society,” he explains.
This mentality causes some men to overlook many other common symptoms such as:
Age, race, and ethnicity, as well as gender identity factor into men’s underuse or avoidance of health and preventive health care, Dr. Scallon says. For example, young men who lack medical issues don’t necessarily need preventative screening but do need attention when it comes to mental health, safety, and behavioral risk-taking. “Young adulthood is where many of us develop lifelong habits, so we need to focus on getting young men accustomed to healthy living, even if they do not see the benefits immediately.”
Race and ethnicity may also play a role in men’s use of preventative health care. “Minority racial groups are less likely to be offered appropriate cancer screenings, even though they have higher risks than other men of developing more aggressive forms of cancer at a younger age,” Dr. Scallon says. “Black and Latino men receive colon and prostate cancer diagnoses at younger ages than white men, yet these cancers have often already spread, which makes treatment more difficult,” he says.
Obesity-related medical issues, such as high blood pressure, diabetes, and high cholesterol frequently go undertreated in minority groups, Dr. Scallon says. “As clinicians, we need to be mindful about how we engage with our patients on these issues and discuss them in ways that creates trust and buy-in for treatment.”
Individuals in sexual minority groups commonly forgo regular health screenings because of past negative interactions with the medical community. But screening is crucial for sexual minority patients, who are more likely than others to experience societal stigma, domestic abuse, or sexual violence, he notes.
Discuss with your primary care physician which health screenings are appropriate for you. Among the most important screenings are those that assess cholesterol, blood pressure, diabetes risk, and weight, which can detect and prevent cardiovascular disease.
At some point, you should also undergo screenings for the following cancers:
Says Dr. Scallon, “All screenings should be discussed with a primary care physician, as family history, age, and other medical issues can affect whether or not they are necessary and beneficial.”