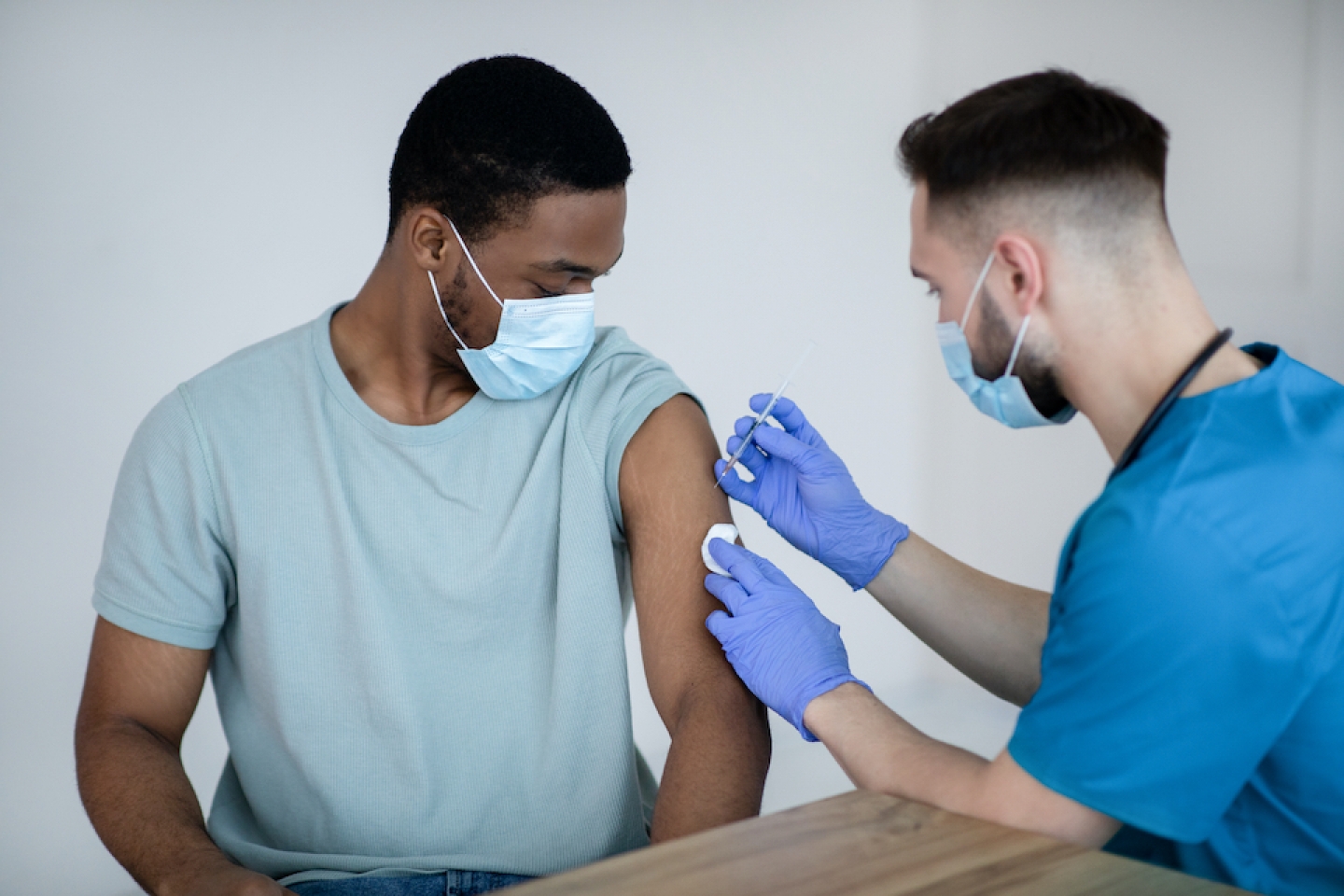
The good news: States are expanding eligibility for the COVID-19 vaccine so rapidly that more than three million people, on average, are receiving a shot each day in the United States, according to the Centers for Disease Control and Prevention.
The less good news: As of April 22, 2021, one in three people in the United States over the age of 18 years were fully vaccinated and more than half of U.S. adults had received at least one dose of a COVID-19 vaccine. This means that we have a way to go to reach the 70% to 85% needed for the United States to achieve herd immunity and stop the disease from spreading.
Why are so many Americans still unvaccinated? And why are rates of vaccination higher in white Americans than in black, Indigenous and people of color (BIPOC)? Among the many reasons is a lack of trust, resulting from America’s long history of unethical treatment of BIPOC in medicine and research, says Linnie M. Golightly, M.D., Associate Dean of Diversity and Inclusion at Weill Cornell Medicine and Associate Professor of Clinical Medicine, Microbiology & Immunology, Division of Infectious Diseases, Center for Global Health.
The most noted example of such mistreatment is the 1932 Tuskegee Study of Untreated Syphilis in the Negro Male, in which the U.S. Public Health Service, together with the Tuskegee Institute, “studied” 600 impoverished African-American men--399 of whom had latent syphilis--to see how the disease progressed and, despite the promise of free medical care, never provided any. Ultimately, 128 study participants died, either directly from syphilis or from related complications.
There are other reasons for leeriness about the shot, including: religious prohibitions against vaccinations; concern about vaccine safety among pregnant and breastfeeding women, as well as individuals with chronic health conditions; the ‘anti-vaxxer’ movement, which opposes vaccination generally; as well as the speed of the vaccine’s development. “There’s an overall fear of both COVID-19 and the vaccine,” Dr. Golightly says. “Here’s a new disease that people had never heard of before 2020, and now almost everyone knows someone who has died from it.” People are afraid of both the disease and the cure.
Yet, widespread trust in the vaccine is critical for creating the level of immunity needed to halt the spread of COVID-19 and its variants. This calls for education, Dr. Golightly says. “If you educate people, then they are empowered to personally make a decision to take it, and the more people who take it, the more people will perceive it as safe.”
Here’s how you can educate yourself:
For example, Pfizer BioEnTech and Moderna produced their vaccines as fast as they did because the messenger RNA (mRNA) engineering used to make them was already in development. “They were easy to make because scientists already had the template. No steps were missed,” Dr. Golightly says.
Emergency Use Authorization (EUA) is a mechanism that the U.S. Food and Drug Administration (FDA) uses to make medical treatments, such as vaccines, available during public health emergencies. Issuing an EUA requires adequate manufacturing information that ensures quality and consistency, and that the vaccine’s benefits outweigh its risks.
Read the packaging or go online to find out what’s in the vaccines. You can also ask your doctor or pharmacist. “Patients should be empowered to look at the vaccine’s ingredients,” Dr. Golightly explains. “No one should be discouraged from trying to understand what’s in the vaccine.”
Because they do not contain live virus, they cannot infect you with COVID-19. In very rare cases, people have experienced serious allergic reactions to the vaccine, and these have generally occurred in individuals with a history of serious allergic reactions. So long as you are not allergic to any of the vaccine’s ingredients, and any medications that you take do not interact negatively with it, then you can safely take it. Another rare side effect--the development of blood clots--has occurred in an extraordinarily small number of patients who received either the Johnson & Johnson or Oxford-AstraZeneca vaccine. The U.S. Food and Drug Administration has not yet authorized use of the AstraZeneca-Oxford vaccine. It recently ended a temporary pause in usage of the Johnson & Johnson vaccine, with the requirement that package labeling include warning about the possibility of blood clots. “Based on the knowledge we have now and the risk of disease, most people would be better off with the vaccine than risking the virus,” Dr. Golightly says.
If you have a history of severe allergic reactions or anaphylaxis, then consult your primary care physician or allergist. “People who have a history of anaphylaxis should carry their EpiPens,” Dr. Golightly says.
If you have a particular medical condition, like lupus or some other immunodeficiency, or cancer, then talk to your medical specialist about the potential risks and benefits of vaccination. You might find information from the organization that researches your condition, such as the Lupus Research Alliance or the American Cancer Society. “I don’t know of any major medical organization that has said ‘Do not get the vaccine,’” Dr. Golightly says.
If you are immunocompromised, you are at increased risk for dying from severe COVID-19, which is why the CDC urges you to get the shot. Studies excluded immunocompromised patients because they believed that the vaccine would not work as well in them as in other patients, given their weakened immune response, Dr. Golightly says.
If you are pregnant or breastfeeding, there is no biologic reason to suspect that the vaccine would be unsafe, says Laura E. Riley, MD, chair of Obstetrics and Gynecology at Weill Cornell Medicine and Given Foundation Professor in Clinical Obstetrics and Gynecology, who help draft The American College of Obstetricians and Gynecologists’ (ACOG) initial guidance for COVID-19 vaccine use for pregnant and lactating patients. “Although data on these patients isn’t yet available, we do know that COVID-19 disease in pregnant women is associated with greater risk for severe illness leading to ICU admission and need for mechanical ventilation,” Dr. Riley says. She notes that pregnant patients should have access to vaccine trial data and speak with their ob-gyn about vaccine efficacy, its benefits, risks, and potential side effects for mothers and their fetus or newborn, as well as virus risks and transmission rate in their community.
If you oppose taking a vaccine whose research and development involved fetal cells, then you can choose one that did not involve fetal cell use. “See what is being said in your religious community,” Dr. Golightly says. Most religious leaders are advising that people should receive one of the vaccines.
Visit the CDC and National Medical Association (NMA) websites. The NMA is the oldest and largest organization representing more than 30,000 African-American physicians and health professionals, and their patients. “Recognizing that there would be concerns about vaccine safety and trust in the Black community, the NMA established a committee to review clinical trial data,” Dr. Golightly says, urging people to look at their findings. “So far, the NMA supports the use of the Moderna and Pfizer vaccines but has not yet issued an opinion about the Johnson & Johnson vaccine.”
“When someone you trust gives you information, then you can hear it, especially if you’re armed with your own information.”
Remember that you are in control. The decision to get vaccinated is yours. Educate yourself. “Patients have the power to look up information and make an informed decision,” Dr. Golightly says.