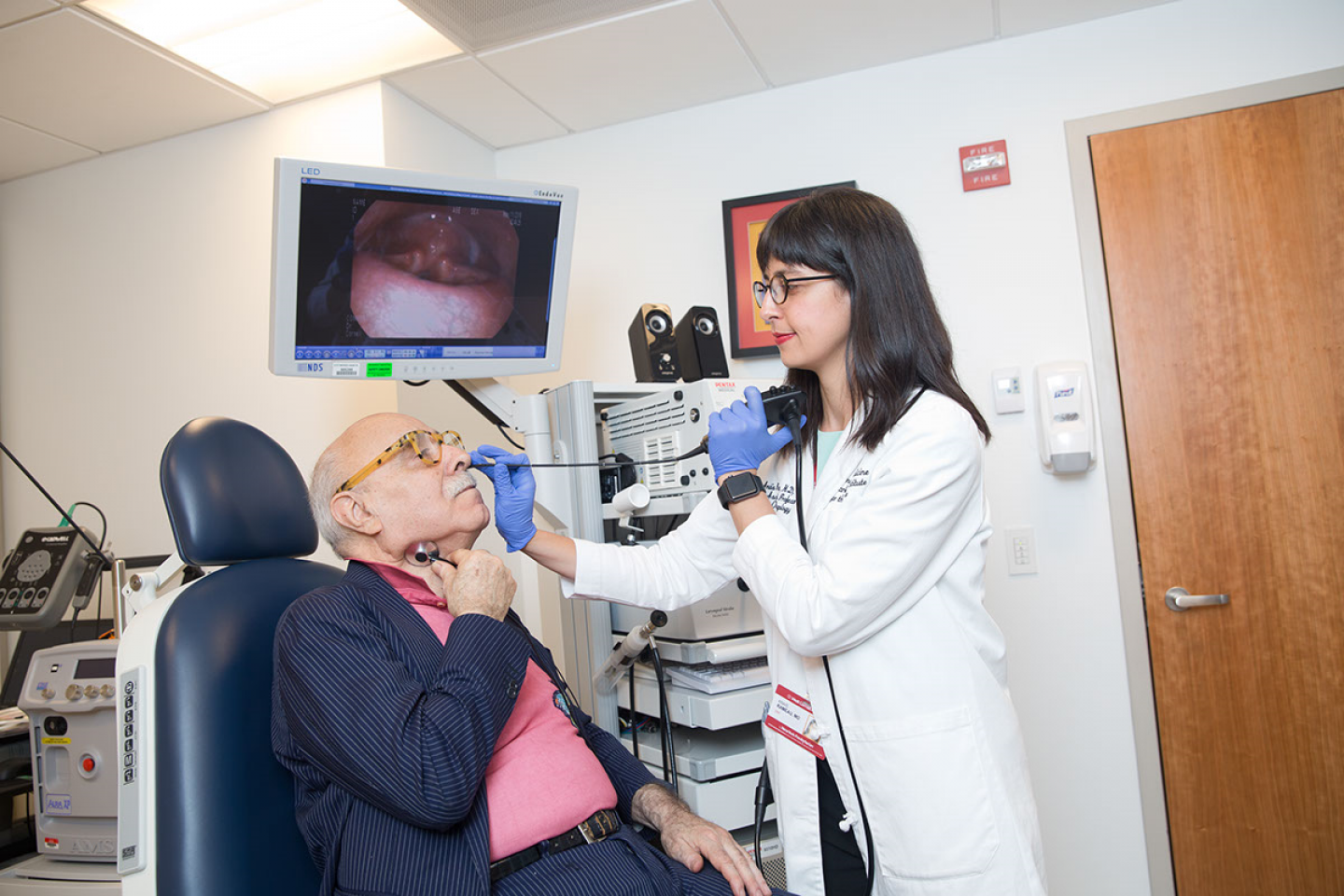
One of the most effective and essential diagnostic tools an otolaryngologist has to examine patients suffering from hoarseness is the laryngoscopy—in shorthand, “scoping.”
Sometimes patients express anxiety about the procedure. Lucian Sulica, MD, director of the Sean Parker Institute for the Voice, explains what patients really need to know about laryngoscopy.
The laryngoscopy is a procedure used to see the vocal folds and neighboring tissue in the larynx or other parts of the throat.
There are two levels to this procedure. The first involves the physician passing a thin, flexible tube with a fiber optic cable on it from the nose to the vocal folds to look for possible abnormalities in the nose, throat, and larynx.
A second, related procedure—one that’s helpful when we’re examining people whose work involves heavy vocal use—is called a stroboscopy. It gives us a finer diagnosis than the laryngoscopy. During a stroboscopy, we apply a a microphone to the skin of the neck overlying the larynx to register the frequency of the voice. This is connected to a strobe light, which flashes slightly out of sync with the frequency, offering a video image of the vocal fold’s vibration.
Yes—we use a local anesthetic spray that quickly numbs the area where the thin tube will pass. It’s done right in the doctor’s office.
Once the patient is numb, we carefully guide the tube down to the vocal folds. Then the doctor will ask the patient to do a few vocal tasks (we may ask a performer to sing a piece they’ve been struggling with, for example) to make an accurate evaluation.
We can make a diagnosis on the spot—this straightforward procedure is the lynchpin in developing an effective treatment plan. In about three minutes, we can conduct a very thorough exam.
Sometimes people feel there will be a risk to undergoing a laryngoscopy. In my experience, once in a great while, a patient will get a nosebleed.
Some patients are concerned about what we’ll find. From performers to attorneys to salespeople, some mistakenly assume that a vocal fold injury diagnosis will be career-ending. Headlines sometimes catastrophizing these injuries don’t help.
It’s also not helpful that people sometimes blame the patient, or the patient will blame themself, but these injuries are typically just a product of hard work.
Here’s the truth: most people with vocal fold injuries don’t require surgery. Behavior management such as voice therapy is helpful and available at the institute. For those patients who do require surgery, most return to work in top form.
In fact, the true risk here is for patients to avoid being evaluated.